[ad_1]
In a recent study published in eBioMedicine, researchers investigated whether human umbilical cord-derived mesenchymal stem cells (hUC-MSCs) could heal luminal ulcers in Crohn’s disease (CD) patients.
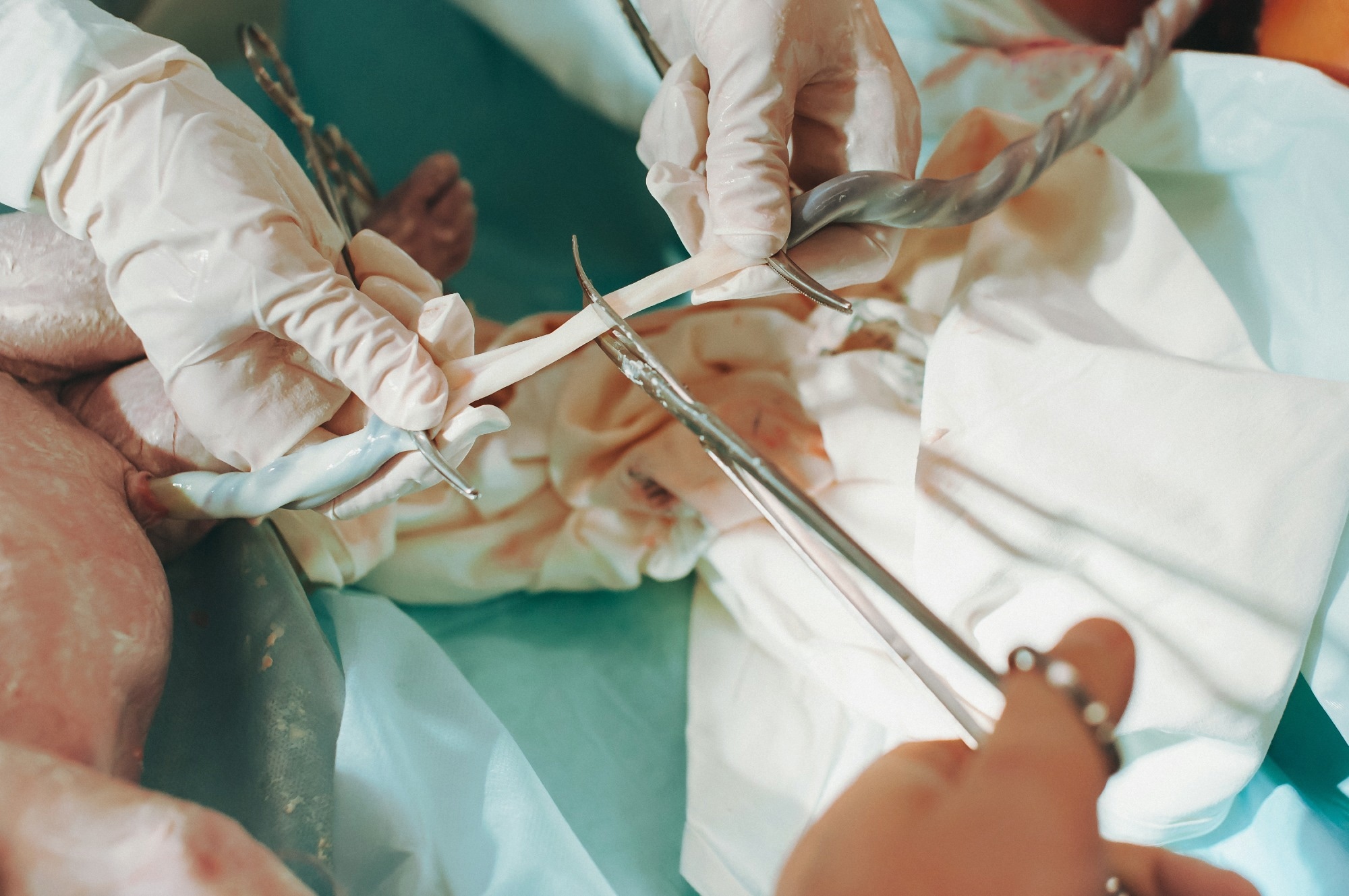 Study: hUC-MSCs therapy for Crohn’s disease: efficacy in TNBS-induced colitis in rats and pilot clinical study. Image Credit: Lobachad/Shutterstok.com
Study: hUC-MSCs therapy for Crohn’s disease: efficacy in TNBS-induced colitis in rats and pilot clinical study. Image Credit: Lobachad/Shutterstok.com
Background
CD is a developing global disease with a poor overall effectiveness rate, posing a considerable therapeutic challenge to health professionals. Current therapies have limitations, and recovery rates are far from expected.
MSC-based therapy has demonstrated promise as a potential new treatment option for various disorders, including CD of the perianal fistulizing type. However, limited evidence is available on the efficacy of MSCs in treating or healing intestinal ulcers in CD.
Human umbilical cord MSCs have acquired popularity due to their immunomodulatory capabilities, simplicity of collection, limitless source of stem cells, low immunological rejection, and lack of tumorigenic features.
Despite their usefulness in immunological and inflammatory illnesses, there has been no research on using hUC-MSCs locally to heal intestinal ulcers in CD patients.
About the study
The present study researchers explored hUC-MSC safety and effectiveness in CD management.
The researchers used the 4,6-trinitrobenzene-sulfonic acid (TNBS)-inflicted colitis rat model to investigate the effectiveness of hUC-MSC therapy in CD. They calculated the disease activity index (DAI) by adding values for body weight loss, stool consistency, and stool blood.
The colon macroscopic damage index (CMDI) assessed the level of colonic inflammation. They analyzed colon samples under a microscope to establish histopathological scores (HPS).
From November 2020 to October 2023, the researchers ran a pilot, open-label clinical study with 17 refractory CD patients. Participants received a local submucosal injection of hUC-MSCs (60 × 106 cells/10 mL) by colonoscopy, followed by an intravenous drip of 1.0 × 106 hUC-MSCs/kg/100 mL the following day.
The study included individuals aged 18–75 years with moderate-severe CD for ≥3 months, baseline CDAI scores of 220-450, and endoscopic ulcers. They did not respond to conventional or advanced treatment, including immunomodulators and biologics.
The researchers followed the patients for 24 weeks, measuring laboratory and clinical markers on days 0, week 4, week 8, week 12, and week 24.
They performed endoscopic assessments at the start of the trial and, after 12 weeks, obtained mucosal specimens from lesion margins for ribonucleic acid (RNA) sequencing. The researchers excluded individuals with a history of pregnancy, CD complications, comorbidities, prior surgery, uncontrolled infections, or cancer in the past five years.
The team also produced two hUC-MSC in vitro co-cultures using mucosal tissues and the human monocyte cell line THP-1-induced M1 macrophages. Reverse transcription-polymerase chain reaction (RT-PCR) measured inflammatory and intestinal barrier function-related genes.
In addition, the researchers performed gene ontology (GO) analysis and explored the Kyoto Encyclopedia of Genes and Genomes (KEGG) pathway enrichment.
They used enzyme-linked immunosorbent assays (ELISA) to assess the expression of tumor necrosis factor-stimulated gene-6 protein (TSG-6) in hUC-MSC culture supernatants after 48 hours of stimulation with lipopolysaccharide (LPS), interferon-gamma (IFNγ), and TNF-alpha (TNFα) for 48 hours.
Results
In preclinical studies, hUC-MSCs raised body weight while decreasing DAI, CMDI, and HPS scores in the TNBS-inflicted colitis murine model, with significant reductions in intestinal mucosal injury, edema, hyperemia, and ulcerations.
Local and submucosal hUC-MSC injections resulted in intestinal ulcer regression in the study participants.
Among the subjects, eight (47%) displayed endoscopic responses (a ≥50% improvement in SES-CD scores), and three (18%) demonstrated mucosal healing, with parallel improvements of laboratory and clinical markers without significant side effects.
Human umbilical cord-derived MSCs increased transcripts associated with intestinal barrier integrity while decreasing those related to inflammatory intestinal mucosal pathways, including TNF-α, interleukin-17 (IL-17), and toll-like receptor (TLR) signaling.
The treatment dramatically enhanced RNA levels of tight junction proteins [E-cadherin (CDH1), zonula occludens-1 (ZO1), and claudin-1 (CLDN1)] in the intestinal epithelium and intestinal pro-inflammatory genes (TNF-α, IL-1β, and IL-6).
Furthermore, hUC-MSCs reduced THP1-induced M1 macrophage polarization and messenger RNA (mRNA) expressions of TNF-α, IL-1β, and IL-6.
MSCs obtained from the human umbilical cord suppressed Janus kinase/signal transducers and activators of transcription (JAK/STAT) phosphorylation in intestinal mucosal cells from Crohn’s disease patients.
Conclusions
The study findings showed that submucosal injection of hUC-MSCs by colonoscopy, paired with an intravenous drip, reduced TNBS-inflicted colitis among rats. This technique may treat refractory CD with clinical effectiveness and tolerable risk.
TSG-6 release may contribute to the therapeutic effect by inhibiting JAK/STAT phosphorylation, reducing M1 macrophage polarization, and improving intestinal barrier function.
In individuals with moderately or highly active CD, hUC-MSC treatment resulted in clinical remission and the repair of intestinal ulcers.
The expression of STAT1, M1 macrophage-associated specific markers, and pro-inflammatory factors in the intestinal mucosa dropped considerably following therapy. Further research is required to establish the efficacy of hUC-MSC treatment and investigate the underlying processes of the therapy.
[ad_2]
Source link