[ad_1]
In a recent study published in the Journal of American Medical Association (JAMA), researchers from the United States of America (US) compared the safety, efficacy, and long-term outcomes of bariatric surgery and medical and lifestyle management in patients with type 2 diabetes mellitus (T2DM). They found that patients undergoing bariatric surgery had better glycemic control and higher remission rates at 7–12 years compared to medical management.
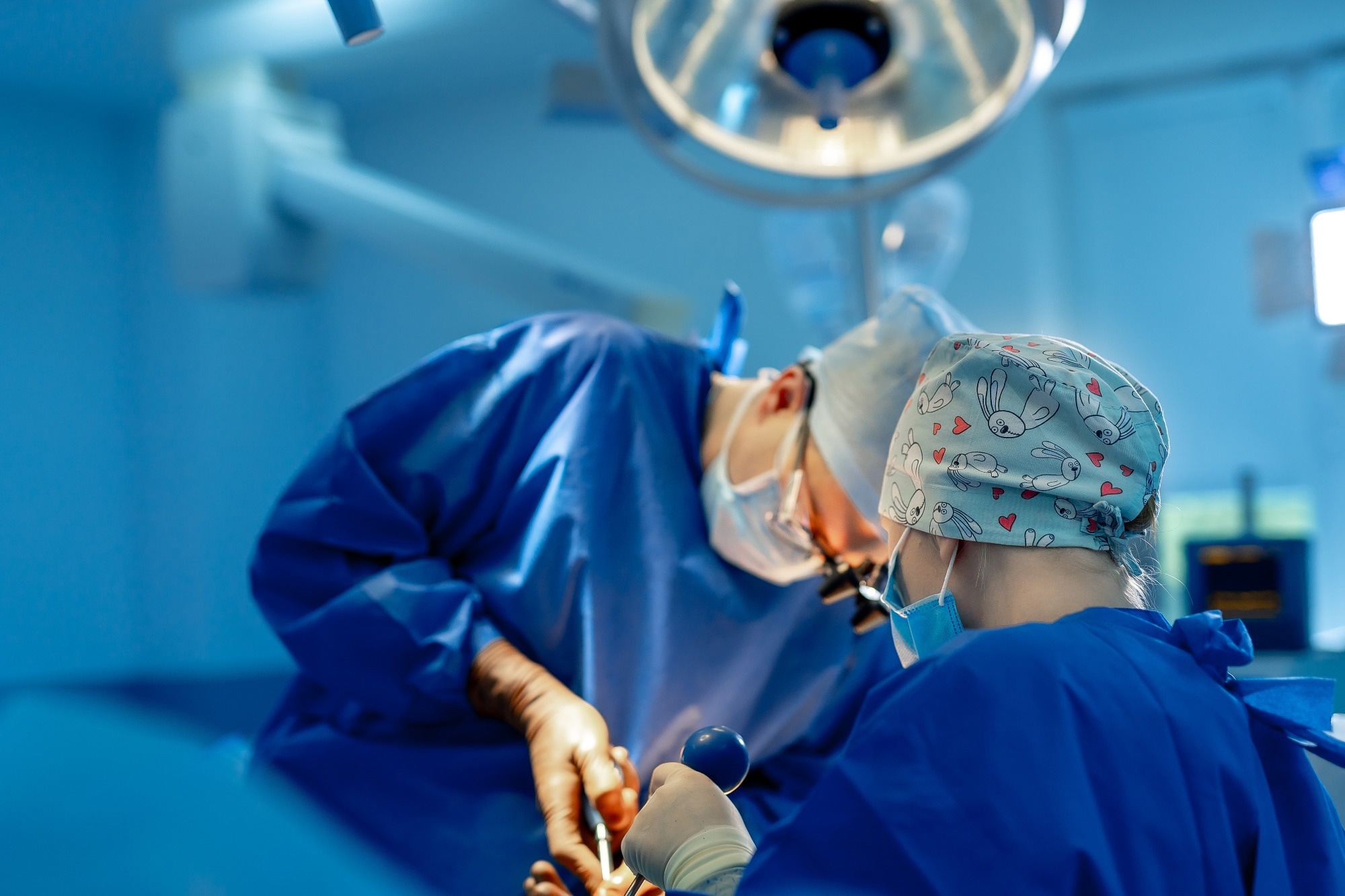 Study: Long-Term Outcomes of Medical Management vs Bariatric Surgery in Type 2 Diabetes. Image Credit: Terelyuk / Shutterstock
Study: Long-Term Outcomes of Medical Management vs Bariatric Surgery in Type 2 Diabetes. Image Credit: Terelyuk / Shutterstock
Background
T2DM affects over 500 million adults globally, presenting significant economic burdens. Although bariatric surgery has shown superiority over medical and lifestyle therapies in treating the condition, limited randomized controlled trials (RCTs) with constraints in sample size and follow-up duration have hindered widespread recommendations. This has led to less than 1% of individuals with a body mass index (BMI) of 35 kg/m2 or higher considering surgical treatment. Despite advances in weight loss medications, their cost, uncertain long-term efficacy, and the need for prolonged use pose challenges.
The Alliance of Randomized Trials of Medicine vs. Metabolic Surgery in Type 2 Diabetes (ARMMS-T2D) consortium conducted the most extensive pooled analysis to date, combining long-term observational data from four US single-center randomized trials. It aimed to assess bariatric surgery’s safety, durability, and efficacy compared to medical/lifestyle treatment for T2DM. At three years, the study revealed the superior and sustained effectiveness of bariatric surgery over medical/lifestyle intervention, even in individuals with a BMI of 25–35 kg/m2. In the present study, researchers report the extended follow-up results at 7–12 years after randomization.
About the study
The study included 262 T2DM patients with a BMI of 27–45 kg/m2. The mean age was 49.9 years, and 68.3% of them were female. Patients were randomized to undergo intensive medical and lifestyle management (n = 96), or bariatric surgery (Roux-en-Y gastric bypass, sleeve gastrectomy, or adjustable gastric banding), and postoperative care (n =166). Based on self-reported racial information, about 31% of patients were Black, and 67.2% were White. While the study was conducted between 2007 and 2013, the observational follow-up was conducted until 2022.
The study’s primary outcome was a between-group difference in the change (%) in glycated hemoglobin (HbA1c) from baseline to seven years, with extended data up to 12 years. The secondary outcomes were changes in HbA1c, changes in various metabolic and cardiovascular parameters, and diabetes remission, with a hypothesis favoring bariatric surgery over medical/lifestyle treatment. Adverse events were systematically collected, covering serious events and complications up to 12 years. The statistical methods involved the use of a linear mixed-effect model, inverse probability weighting, sensitivity analysis, and exploratory analyses.
Results and discussion
In spite of higher baseline values, the bariatric surgery group consistently maintained significantly lower HbA1c levels than the medical group, with a difference of -1.4% and -1.1% at seven years and 12 years, respectively. At seven years, HbA1c improvements were similar between Roux-en-Y gastric bypass and sleeve gastrectomy, while adjustable gastric banding showed less improvement than sleeve gastrectomy (P = .007) and Roux-en-Y gastric bypass (P = .03). As 25% of patients switched from medical management to surgery during the study, a per-protocol sensitivity analysis was conducted, which confirmed the main results.
At one year, diabetes remission was achieved by 0.5% of patients in the medical group as compared to 50.8% in the surgery group. At seven years, remission rates were 6.2% vs. 18.2% in the medical group and surgery group, respectively, and the difference persisted at 12 years. HbA1c was found to be < 7% in 26.7% of patients in the medical group vs. 54.1% of those in the surgery group. Additionally, bariatric surgery resulted in significantly higher weight loss and rates of non-obesity at 7 and 12 years. The surgery group also experienced significantly reduced medication and insulin use as compared to the medical group. Further, the bariatric group showed significantly higher high-density lipoprotein (HDL) and lower triglycerides. No significant differences were observed for systolic blood pressure, low-density lipoprotein (LDL), serum creatinine, or urine albumin-to-creatinine ratio in the two groups at seven years. Adverse events were found to be similar between the groups, with increased gastrointestinal events in the surgery group.
The study is strengthened by its larger sample size, diversity in sampling, inclusion of data on the most common surgical procedures, and longer follow-up compared to previous studies. However, the study is limited by its open-label design, heterogeneous treatments, missing data, lack of power for procedure-specific outcomes, and changes in surgical procedures and medication use during follow-up.
Conclusion
In conclusion, after 7 to 12 years, patients assigned to bariatric surgery demonstrated better glycemic control, reduced diabetes medication usage, and higher rates of diabetes remission compared to those on medical/lifestyle intervention. The findings endorse the employment of bariatric surgery as a viable treatment option for T2DM in individuals with obesity.
[ad_2]
Source link